Healthcare has undergone massive digital transformation over the past decade. Electronic health records (EHRs), telemedicine platforms, and digital prescribing systems were introduced to streamline care and improve data accessibility. Yet many clinicians argue that one critical process has become more time-consuming than ever: clinical documentation.
As healthcare systems increasingly struggle with documentation overload, many providers are turning to advanced digital solutions powered by artificial intelligence. Partnering with an ai app development company in usa enables healthcare organizations to build tailored tools such as automated clinical note generation, voice-to-text transcription, and intelligent EHR integrations. These AI-driven applications not only reduce administrative burden but also improve accuracy and efficiency, allowing clinicians to focus more on patient care rather than paperwork.
What was originally meant to improve record-keeping has unintentionally created a major administrative burden. Physicians, physiotherapists, and other healthcare providers now spend a significant portion of their day entering notes, updating patient charts, and ensuring records meet regulatory standards.
As healthcare systems continue to scale and patient volumes rise, documentation is increasingly being recognized as one of the biggest workflow bottlenecks in modern medicine.
The Documentation Burden Is Growing Across Healthcare Fields
Clinical documentation is essential. Accurate notes allow healthcare professionals to track patient progress, communicate with colleagues, and maintain compliance with legal and billing requirements.
However, the process itself often disrupts the clinical workflow.
Recent studies have shown that many physicians spend nearly two hours on documentation for every hour spent with patients. In some cases, clinicians complete notes after hours, a phenomenon commonly referred to as “pajama time.”
The issue is not limited to physicians. Many other healthcare professionals experience similar challenges:
- Physiotherapists documenting treatment progress and rehabilitation plans
- Mental health providers recording therapy sessions
- Nurse practitioners managing complex patient histories
- Specialists maintaining detailed diagnostic notes
While documentation improves continuity of care, the growing administrative load can reduce time available for direct patient interaction.
Why Traditional Documentation Methods Are Inefficient
Historically, clinicians dictated notes or wrote them manually. With the rise of EHR systems, documentation became digital but also more structured and compliance-driven.
This shift introduced several inefficiencies:
1. Structured forms require repetitive data entry
Many electronic records require clinicians to manually input information that may already be mentioned during the patient consultation.
2. Note creation happens after the visit
Clinicians frequently document encounters after the patient has left, forcing them to recall details from memory.
3. Administrative workflows interrupt care
Switching between patient interaction and typing notes often breaks the natural flow of the consultation.
Over time, these inefficiencies compound, leading to clinician fatigue and longer workdays.
The Rising Role of AI in Clinical Documentation
Artificial intelligence is increasingly being explored as a solution to the documentation burden.
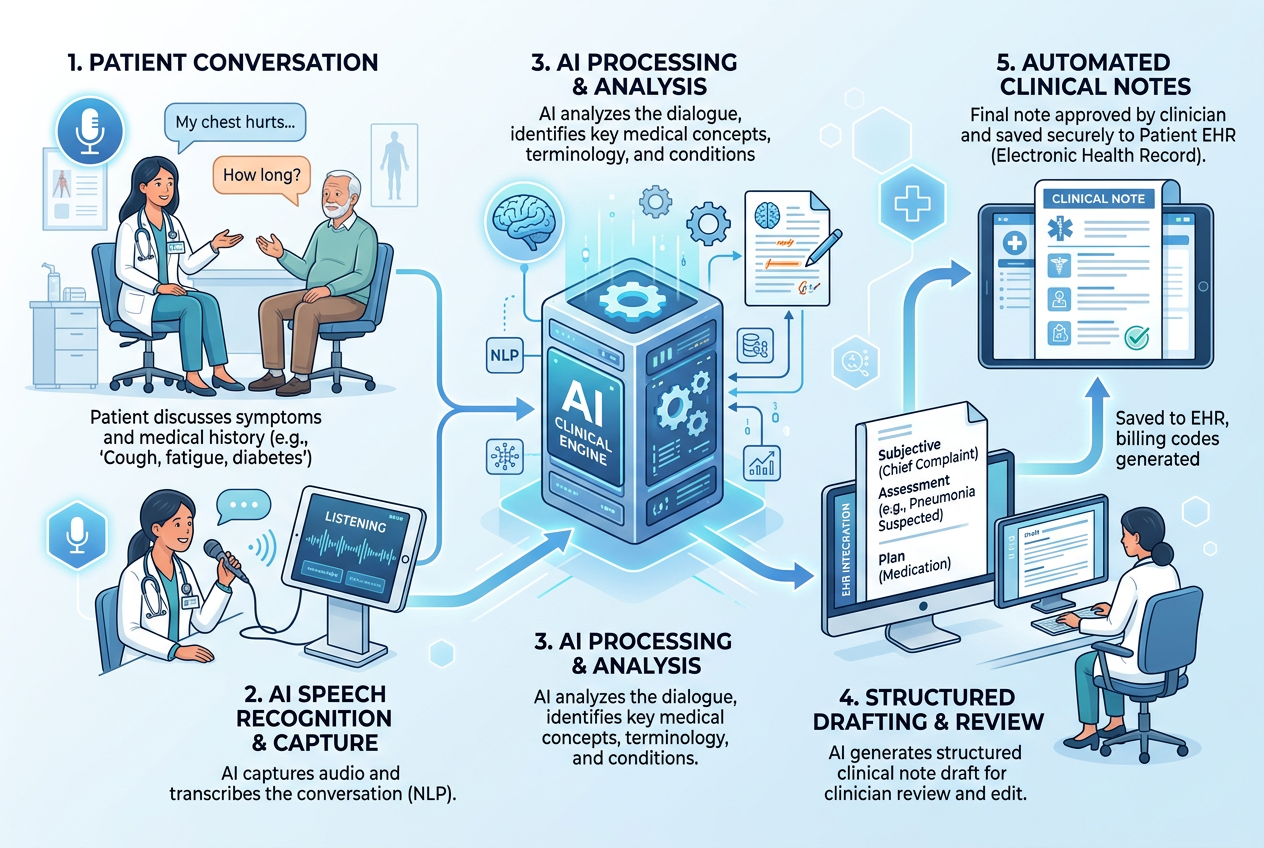
Modern healthcare AI systems can analyze conversations between clinicians and patients, extract relevant information, and generate structured notes that fit clinical documentation standards.
Solutions built around AI clinical documentation are beginning to reshape how healthcare professionals manage their notes. These systems capture conversations during consultations, identify medically relevant details, and transform them into structured clinical documentation that can be quickly reviewed and finalized by the clinician.
Rather than replacing healthcare professionals, these tools act as intelligent assistants that help convert natural conversations into organized medical records.
The goal is not automation for its own sake but workflow optimization. When documentation happens seamlessly during the consultation, clinicians can focus more on the patient rather than the keyboard.
How AI Documentation Assistants Improve Clinical Workflows
Healthcare organizations experimenting with AI documentation tools are seeing several operational benefits.
Reduced Administrative Time
Automated note generation allows clinicians to spend less time writing reports after appointments.
More Accurate Clinical Notes
AI systems can capture details in real time, reducing the likelihood of forgetting information after a consultation ends.
Improved Patient Engagement
When clinicians do not need to constantly type during a visit, they can maintain better eye contact and communication with patients.
Faster Chart Completion
Many clinicians are able to finalize documentation immediately after reviewing AI-generated notes, eliminating hours of end-of-day paperwork.
While adoption is still evolving, these tools are increasingly viewed as a practical solution to documentation overload.
The Future of Clinical Documentation
Healthcare documentation will continue to evolve alongside advancements in artificial intelligence, natural language processing, and speech recognition technologies.
Future systems will likely integrate directly into clinical workflows, automatically generating structured documentation, extracting medical insights, and supporting decision-making processes.
As healthcare systems face growing patient demand and clinician shortages, reducing administrative friction will become increasingly important.
Clinical documentation will always remain a core part of healthcare practice. However, the way it is created is rapidly changing, and intelligent documentation tools may soon become a standard component of modern medical workflows.











Comments