Within the field of psychodermatology lies a complex condition where physical signs stem from psychological needs. This psychocutaneous disorder involves the deliberate creation of bodily injuries.
Individuals with this presentation have full awareness of their actions. They consciously produce damage to their skin, hair, nails, or mucous membranes. Yet, they consistently conceal their role from clinicians.
This behaviour distinguishes it from other forms of deliberate self-harm. In those situations, patients often acknowledge their responsibility. Here, the denial is a core, defining feature.
The situation presents a significant clinical puzzle. It sits at the unique intersection of dermatological presentation and psychiatric aetiology. Effective management demands integrated expertise from both specialities.
Healthcare professionals must approach these patients with sensitivity and a high index of suspicion. The manifestations are real, even if their origin is consciously obscured. Understanding this dynamic is the first step towards appropriate care.
Key Takeaways
- Dermatitis artefacta is a psychocutaneous disorder where individuals deliberately create their own physical injuries.
- Those affected have full insight into their actions but deny any responsibility for causing the damage.
- This condition differs from other self-harm behaviours, where acknowledgement of the act is more common.
- It requires a collaborative approach between dermatology and psychiatry for accurate diagnosis and management.
- The clinical presentation can involve the skin, hair, nails, or mucous membranes.
- Diagnosis is challenging due to the patient’s conscious concealment of the behaviour.
- It should be considered in cases of chronic, unexplained, or recurrent dermatological issues.
Introduction to Dermatitis Artefacta
Defining this condition requires understanding both its dermatological appearance and psychiatric drivers. Known alternatively as factitious dermatitis, it is a rare psychocutaneous disorder. Individuals consciously produce damage to their own body.
They seek no external reward, unlike in malingering. The act fulfils an internal psychological need, often for attention or care. This is a core aspect of dermatitis artefacta.
Defining the Condition
The defining feature is conscious creation paired with denial. Patients have insight but conceal their role. This creates a significant diagnostic challenge for the disorder.
Psychiatric and Dermatological Perspectives
From a dermatological view, lesions appear bizarre. They often mimic inflammation and occur on accessible areas. Patterns defy typical disease classifications.
Psychiatrically, the behaviour reflects underlying emotional distress. It may relate to personality disorders, depression, or neuroses. The cutaneous damage is a somatic expression of this distress.
Successful management hinges on collaboration between dermatology and psychiatry. Neither specialty alone holds all answers. An integrated approach is essential for care.
Clinical Overview and Historical Context
Tracing the clinical history of this condition reveals a fascinating journey from isolated case observations to systematic international reviews. Medical comprehension has evolved through documented cases and accumulating evidence.
Evolution of the Diagnosis
A pivotal moment occurred with the 1975 work of Sneddon and Sneddon, often cited as the first major systematic report. Early focus was on the strange appearance of injuries and inconsistent patient narratives.
Diagnostic thinking later deepened. It moved beyond noting physical signs to exploring complex psychological drivers. This shift marked significant progress in psychiatric sophistication.
“Historical case studies provide the essential clinical bedrock upon which our modern diagnostic frameworks are built.”
Historical Case Reports
Foundational reports emerged from the United Kingdom, Switzerland, and beyond. These early studies described the presentation across diverse cultures, confirming it was not region-specific.
Subsequent international cases from Saudi Arabia, Mexico, India, and European nations built a robust global picture. They highlighted both universal features and subtle cultural variations.
|
Region/Country |
Notable Finding from Historical Data |
Clinical Implication |
|
UK & Switzerland |
Provided initial detailed descriptions of lesion morphology and patient denial. |
Established core, recognisable clinical patterns for clinicians. |
|
International Series (e.g., Iran, Spain, Poland) |
Documented the condition’s presence across continents. |
Proved dermatitis artefacta transcends cultural and geographic boundaries. |
|
Demographic Analyses |
Aggregate data showed a strong female preponderance (~81%). |
Highlighted a key risk group, typically adolescents and young adults. |
This collective history of over 330 assessed patients solidified understanding. It revealed important subgroups and set the stage for today’s integrated management strategies.
Understanding Dermatitis Artefacta: Self-Inflicted Skin Lesions in Psychiatric Contexts
Healthcare professionals encounter a scenario where the skin tells a story the patient cannot verbalise. The visible damage acts as a physical expression of deep, internal psychological conflict. It is a maladaptive coping mechanism where distress is communicated through the body.
The psychiatric background varies widely. It spans from transient stress in emotionally immature individuals to severe, chronic conditions like personality disorders or major depression. This spectrum is crucial for accurate clinical understanding.
Presentations differ significantly by age. Younger people often exhibit this behaviour as a ‘cry for help’ amidst communication difficulties or family strife. Adults typically have more complex, entrenched psychopathology driving the actions.
|
Feature |
Younger Populations (Children/Adolescents) |
Adults |
|
Typical Presentation |
Often reactive to immediate psychosocial stress (e.g., bullying, academic pressure). |
Reflects long-standing personality patterns or chronic mood disorders. |
|
Common Underlying Drivers |
Anxiety, immature coping styles, family dysfunction. |
Neurosis, depression, impulsiveness, or disturbed interpersonal relations. |
|
Primary Psychological Function |
Non-verbal plea for attention and care. |
Assumption of a ‘sick role’ to avoid responsibilities or express self-directed anger. |
Recognising this diverse psychiatric landscape is why empathetic, non-confrontational care succeeds. Treatment must address the root cause, not just the visible lesions.
Aetiology and Psychopathological Factors
A systematic review of the evidence reveals that nearly half of all individuals with this condition have a co-occurring mental health diagnosis. Understanding these underlying factors is crucial for moving beyond symptom management.
The behaviour is rarely isolated. It typically exists within a broader landscape of psychological distress.
Underlying Psychiatric Disorders
Research indicates 46.2% of patients present with a comorbid psychiatric disorder. Depression is most common, affecting up to one-third of cases.
Other frequent disorders include anxiety and somatoform conditions. Substance use issues are seen in about 18% of patients.
In paediatric cases, intellectual disability is a significant factor. This highlights varied pathways to the same maladaptive coping behaviour.
Emotional and Social Triggers
Significant stressful life events precede symptoms in 40.9% of patients. These triggers differ markedly by age group.
|
Common Triggers |
Younger Populations |
Adults |
|
Psychosocial Stressors |
Academic pressure, bullying, family conflict. |
Occupational stress, relationship breakdown, financial strain. |
|
Underlying Drivers |
Immature coping, peer difficulties. |
Chronic depression, entrenched personality disorders. |
|
Primary Function |
A non-verbal plea for help or attention. |
Assumption of a ‘sick role’ to avoid responsibilities. |
A notable challenge is that 20.1% of patients refuse psychiatric evaluation. This extends the denial seen in clinic.
Recognising these aetiological factors allows for targeted screening. Effective care must address the root cause, not just the visible damage.
Differentiating Dermatological and Psychiatric Presentations
A clear differentiation framework protects against both mislabelling true illness and missing concealed self-harm. This practical guidance helps clinicians separate factitious disorder from organic skin disease and other psychiatric conditions.
Comparative Clinical Features
The morphology of lesions offers the first clue. In dermatitis artefacta, they often appear bizarre, geometric, or linear. They materialise suddenly on accessible body sites, sparing areas the patients cannot reach.
This contrasts sharply with organic conditions like impetigo or contact dermatitis, which follow recognisable patterns. A detailed history is crucial. Clinicians may note a ‘hollow history’ where patients elaborate on treatment failures but are vague about the lesions‘ origin.
“The key is to look for a story that doesn’t fit the physical evidence-lesions that defy anatomy and a narrative full of complications but empty of cause.”
Psychiatric differentiation is equally vital. It is essential to exclude psychotic disorders like delusions of parasitosis. In that condition, individuals genuinely believe parasites cause their symptoms, unlike the conscious concealment in factitious dermatitis.
Clinical Findings and Lesion Characteristics
Clinical examination reveals characteristic injury features and distribution that are key to recognition.
Lesion Morphology and Distribution
The morphology of these presentations is highly variable. Superficial erosions appear in roughly half of all cases.
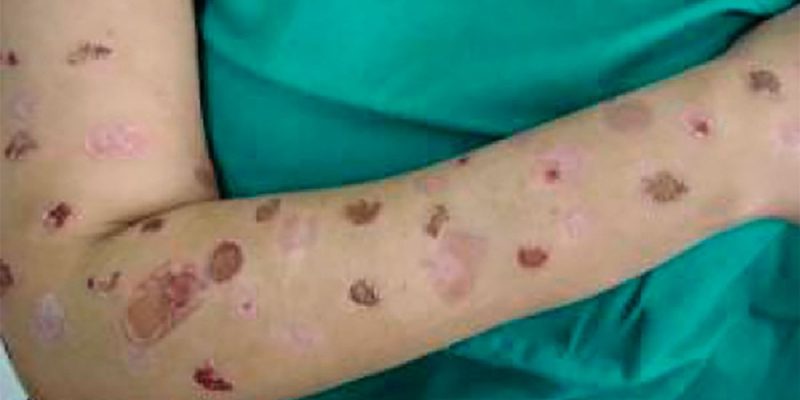
Hyperpigmented macules or purpuric lesions affect 30-42% of patients. Other types include excoriations, papules, crusts, and deep ulceration.
Shapes can be circular, linear, angulated, or in bizarre configurations. These patterns often defy typical dermatological classification.
Distribution follows a telling pattern. The face, particularly the cheeks, is the most common site, especially in children.
The dorsa of the hands and forearms of the non-dominant limb are also frequently involved. This reflects ease of access and manipulation.
A covert pattern exists where damage is hidden under clothing. Involvement of the breasts or genitalia should raise clinical suspicion of underlying trauma or abuse.
Physical versus Psychogenic Signs
Several signs help distinguish these presentations from organic disease. There is often a sharp demarcation between affected and unaffected skin.
Geometric patterns suggest instrumental creation. The surrounding skin typically shows no inflammatory change, unlike many genuine dermatoses.
Most individuals present with multiple injuries of different types and healing stages. This suggests repeated episodes of self-infliction.
Diagnostic Challenges and Differential Diagnosis
The diagnostic process for factitious skin damage is fraught with challenges, primarily due to its overlap with numerous genuine dermatoses. Dermatitis artefacta should be considered in every case of chronic, puzzling, and recurrent skin disease. A systematic approach to differential diagnosis is essential.
Overlapping Dermatological Conditions
Many organic conditions can mimic self-inflicted injury. Crusted or blistering lesions may resemble ecthyma or herpes simplex. More severe presentations can simulate serious disease like porphyria cutanea tarda or cutaneous lymphoma.
Vasculitis, pyoderma gangrenosum, and drug eruptions also enter the differential. This wide range necessitates careful investigation to exclude organic causes.
“The key challenge is to avoid both false positives-labelling real illness as factitious-and false negatives, where self-harm is missed.”
Clinicians must balance thorough exclusion of organic disease against over-investigation. Excessive testing can reinforce illness behaviour. Key clues favouring a diagnosis of dermatitis artefacta include sudden lesion appearance and geometric patterns.
A ‘hollow’ history, where patients are vague on details, is another red flag. Lesions are typically on accessible skin. A non-confrontational approach helps build trust and secure an accurate diagnosis.
Interdisciplinary Approaches and Expert Perspectives
An integrated framework is the cornerstone of effective long-term management for individuals with factitious dermatological presentations. This condition is chronic, and patients require regular follow-up with both a dermatologist and a psychiatrist to manage common relapses.
Collaborative Care Models
Optimal management relies on a dedicated multidisciplinary team. This team typically includes a dermatologist, ideally with psychodermatology training, a psychiatrist or clinical psychologist, and specialist nurses.
This collaborative approach ensures consistent messaging. It prevents patients from receiving contradictory information from different specialists. Needs vary significantly between patient groups.
Some cases resolve with minimal intervention. Others demand intensive, long-term psychological support coordinated by the multidisciplinary team.
Insights from Surgical Arena Ltd
Specialist perspectives are vital in procedural settings. In surgical contexts, non-healing wounds may represent deliberate interference rather than surgical failure.
Protocols established by organisations like Surgical Arena Ltd guide teams. They help in documenting suspicious wound behaviour and implementing protective strategies. The key is to liaise with mental health services rather than pursue repeated surgical treatment.
This interdisciplinary approach respects each specialty’s contribution. It provides the consistent support needed for a disorder with a fluctuating course, improving long-term treatment adherence and overall health outcomes.
Psychological Assessment and Patient History
Skilful history-taking often yields more diagnostic clues than physical examination alone in cases of suspected self-induced injury. A comprehensive psychological assessment is the cornerstone of understanding the individual behind the presentation.
This process requires patience and a non-judgemental approach to build essential trust.
Importance of a Thorough History
The historical narrative is of particular importance. Individuals often describe the sudden appearance of complete, fully-formed marks.
These may appear on waking, with no prodrome or story of development. A detailed account of complications and treatment failure contrasts sharply with vague details about the origin.
This creates a characteristic ‘hollow history’. A good history must extend beyond the skin problem.
It should explore social circumstances, family dynamics, and psychological wellbeing. For a child, separate interviews with parents and the young patient are crucial.
Discrepancies may reveal family dysfunction or unspoken distress.
|
Historical Element |
Typical Presentation in Factitious Cases |
Clinical Implication |
|
Lesion Onset |
Sudden, ‘fully-formed’, often upon waking. |
Suggests deliberate creation, not natural disease progression. |
|
Narrative Focus |
Elaborate on complications; vague on genesis. |
Indicates conscious concealment (‘hollow history’). |
|
Psychosocial Context |
Often reveals current stressors or relational difficulties. |
Highlights potential triggers or secondary gains from the sick role. |
Screening for Comorbid Disorders
Systematic screening for co-occurring mental health disorders is vital. Research shows depression and anxiety are common.
Personality disorders and substance use issues are also frequent. Surprisingly, standard psychometric instruments are rarely used in assessment.
Clinicians should sensitively enquire about life stressors, past psychiatric care, and trauma. Exploring what a patient gains from the behaviour is key.
This assessment is an ongoing process, not a single event. Trust allows for gradual disclosure of underlying difficulties in patients with dermatitis artefacta.
Management Strategies and Treatment Options
The cornerstone of care lies in a coordinated plan that synchronises dermatological support with targeted psychiatric treatment. This dual approach is essential for management of this complex psychocutaneous presentation.
The primary focus must always be on the underlying psychological drivers, not just the visible injuries.
Pharmacological Interventions
Medication aims to treat comorbid psychiatric disorders rather than the lesions directly. Selective serotonin reuptake inhibitors (SSRIs) are first-line for patients with depression or anxiety.
They are often prescribed at the upper therapeutic dose range. Tricyclic antidepressants can help patients experiencing itching, insomnia, or pain alongside low mood.
Low-dose atypical antipsychotics may aid those with marked impulsivity. Prolonged use requires monitoring due to side effects.
Opioid analgesics are avoided to prevent addiction. Non-steroidal anti-inflammatory drugs may be prescribed for symptomatic relief.
Behavioural and Psychological Therapies
Non-pharmacological therapy addresses the behaviour itself. Habit reversal therapy can help if a patient acknowledges damaging their skin.
It involves awareness training and developing competing responses. Cognitive-behavioural therapy targets maladaptive thought patterns and teaches healthier coping.
Barriers include limited service availability and patient reluctance. Realistic goals focus on harm reduction and improving quality of life.
Dermatologists provide wound care, while mental health professionals deliver the core psychological treatment. This clear role specification supports better outcomes for patients.
Case Studies and Clinical Reviews
Insights from aggregated international case reports challenge several long-held assumptions about this psychocutaneous disorder. Synthesising data from multiple sources provides a clearer, evidence-based picture for clinicians.
Lessons from Recent Reviews
A pivotal systematic review analysed 11 studies covering 334 patients across nine nations. A critical lesson is that all included reports were rated as low quality by GRADE criteria.
This highlights a significant research gap. The findings, however, remain instructive. The age range was vast, from two to 86 years.
This dispels the myth that it is solely an adolescent condition. Furthermore, over half of adult patients were married or in stable relationships, contradicting stereotypes of social isolation.
“The international scope of these cases-from Europe to the Middle East-confirms this is a global phenomenon, not bound by culture.”
The review confirmed a strong female preponderance but identified an important subgroup of older males. A major clinical hurdle was the high rate of refusal for psychiatric evaluation.
These studies solidify the need for integrated care. They also expose a lack of randomised treatment trials and long-term outcome data, pointing the way for future research.
Empathy and Non-confrontational Communication
At the heart of effective care lies a simple, yet challenging principle: building trust without confrontation. The quality of the therapeutic relationship fundamentally determines engagement and outcome.
Denial creates inherent barriers. An accepting, empathic attitude is essential from the first consultation.
Building a Trusting Consultation
Accusatory language causes disengagement. Instead, clinicians use indirect phrasing. Suggesting subconscious scratching during sleep preserves dignity while introducing the concept.
Most patients sense the clinician’s understanding. The discussion should then pivot. Framing it around the considerable stress caused by the problem is more productive.
Creating a safe, confidential environment allows underlying difficulties to surface. This non-judgemental approach is the bedrock of care.
|
Communication Strategy |
Effective Approach |
Counterproductive Approach |
|
Addressing Causation |
“There’s no clear medical cause for these marks.” |
“You are doing this to yourself.” |
|
Exploring Impact |
“This must be causing you a lot of distress.” |
Focusing solely on the physical damage. |
|
Managing Non-compliance |
Maintaining open, persistent encouragement for return. |
Expressing frustration or punitive responses. |
Patience is vital. Trust builds over multiple meetings. Clinicians must also manage their own negative feelings to maintain a consistent, supportive relationship. This approach enables the ultimate goal: the patient accepting referral for psychological management.
Incorporating Insights from The Psychodermatologist
The emerging subspecialty of psychodermatology provides a unique framework for clinicians navigating the dual challenges of skin disease and psychological distress. The Psychodermatologist operates at this critical intersection. They bring specialised training in both dermatology and mental health.
This dual expertise allows for a nuanced understanding of dermatitis artefacta. They recognise distinct patient subgroups. For example, experimental or social cases often settle with minimal support.
More complex presentations require intensive, long-term psychological care. A dedicated multidisciplinary team is essential for this. The table below contrasts core principles of this integrated approach with a standard model.
|
Management Aspect |
Standard Dermatological Approach |
Psychodermatological Framework |
|
Primary Focus |
Healing the visible bodily damage. |
Addressing both the physical signs and the underlying psychological suffering simultaneously. |
|
View of Behaviour |
Often seen as manipulative or problematic. |
Understood as maladaptive communication of genuine distress. |
|
Treatment Goal |
Complete resolution of lesions. |
Harm reduction, improved quality of life, and preventing severe complications. |
|
Care Structure |
Episodic dermatology reviews. |
Regular, coordinated follow-up with both dermatology and mental health services. |
These insights are vital even where specialist psychodermatology services are scarce. The core principles-integrated care, compassion, and realistic goals-can guide any clinician managing this long-term disorder. Effective care for these patients hinges on this holistic perspective.
Advances in Research and Future Directions
Emerging studies are shifting focus from broad psychiatric diagnoses to specific cognitive and emotional processes. This new research aims to create more effective treatment plans.
A sensitive, non-confrontational approach remains essential during evaluation. It minimises refusal and improves compliance among patients.
Innovative Therapies and Techniques
Recent review of the literature highlights dissociation and emotion dysregulation as key targets. These mechanisms may be more specific than broad categories like depression.
New therapy models address these directly. Sensorimotor psychotherapy or EMDR may help those experiencing amnesia during episodes.
Dialectical behaviour therapy techniques show promise for emotional modulation. Advances in telepsychiatry could improve access to specialised care.
|
Research Direction |
Current Limitation |
Future Goal |
|
Therapeutic Targets |
Focus on comorbid disorders (e.g., depression). |
Develop interventions for specific mechanisms like dissociation. |
|
Evidence Base |
Reliance on retrospective case series. |
Conduct prospective longitudinal study and randomised trials. |
|
Service Delivery |
Limited access to specialist clinics. |
Use digital platforms for remote consultation and support. |
Future studies must tackle implementation challenges. The goal is practical clinical pathways for all patients, not just those near specialist centres.
Conclusion
Effective care for this psychocutaneous disorder hinges on a compassionate, integrated model. It requires expertise from both dermatology and mental health services working together. This collaborative approach is essential for managing the condition long-term.
Prognosis varies. Mild cases linked to common life stressors often resolve well. Chronic dermatitis artefacta with severe damage has a more guarded outcome. Without proper treatment, risks include serious mutilation and disfiguring scars.
Tragically, suicide is a potential risk for some patients. Treating co-occurring issues like depression can lead to real improvement in the physical marks. Early recognition and intervention are vital.
Ultimately, success relies on non-confrontational support and a multidisciplinary team. Healing must address both the visible injury and the invisible psychological pain. This balanced focus offers the best hope for patients.
FAQ
What is dermatitis artefacta?
Dermatitis artefacta is a condition where an individual deliberately creates lesions on their own skin. This behaviour is linked to underlying psychological distress or mental health disorders, rather than a primary skin disease. The presentation sits at the intersection of dermatology and psychiatry.
What psychiatric issues are commonly associated with this condition?
Patients often have comorbid psychiatric disorders. Common associations include anxiety, depression, and personality disorders. In many cases, the behaviour serves as a maladaptive coping mechanism for emotional pain or unresolved trauma.
How do doctors diagnose this problem?
Diagnosis is challenging and requires a careful, non-confrontational approach. Clinicians rely on a detailed patient history, the unusual morphology and distribution of the lesions (which often do not match known medical conditions), and a high index of suspicion. A multidisciplinary team involving both dermatology and mental health specialists is crucial for an accurate assessment.
What does treatment involve?
Effective management focuses on the underlying psychological causes. Treatment typically involves a combination of approaches, including psychotherapy (such as cognitive behavioural therapy) to address emotional triggers, and sometimes medication for co-existing conditions like depression. The primary goal is to help the patient develop healthier coping strategies.
Can children and adolescents develop this condition?
Yes, although it is more frequently reported in young to middle-aged adults, cases do occur in younger age groups. In children and adolescents, the behaviour is often a manifestation of severe emotional distress or family dysfunction, necessitating a sensitive and family-inclusive management strategy.
Why is a multidisciplinary team important in care?
A collaborative care model is essential because the condition has both physical and profound psychological aspects. Dermatologists can manage the skin damage, while psychiatrists or psychologists address the root mental health disorder. This integrated approach, supported by specialists like those at Surgical Arena Ltd, offers the best chance for long-term improvement.
What is the role of a psychodermatologist?
A psychodermatologist, such as the expert behind the resource The Psychodermatologist, specialises in the relationship between skin and mind. They are uniquely skilled in diagnosing and managing complex cases where psychological factors manifest as physical symptoms, providing tailored therapy and bridging the gap between two medical specialities.












Comments